The 2026 AI Radiography Report: How Machine Learning is Reducing Diagnostic Errors
As artificial intelligence transitions from an emerging novelty to a clinical staple, radiographic diagnosis stands at the forefront of a technological revolution. Industry reports indicate a significant reduction in diagnostic discrepancies across modern dental practices adopting machine learning overlays.
The Dawn of Algorithmic Diagnostics
Over the past half-decade, the conversation surrounding artificial intelligence in healthcare has matured rapidly. In dental medicine, the focal point of this transformation is radiography. For generations, interpreting bitewings and periapical images required an exceptionally trained eye, often susceptible to fatigue, lighting conditions, and cognitive bias. In 2026, the diagnostic paradigm is fundamentally different. Machine learning models, trained on millions of annotated radiographs, now function as tireless "second opinions," instantly highlighting areas of concern that might escape immediate human detection.
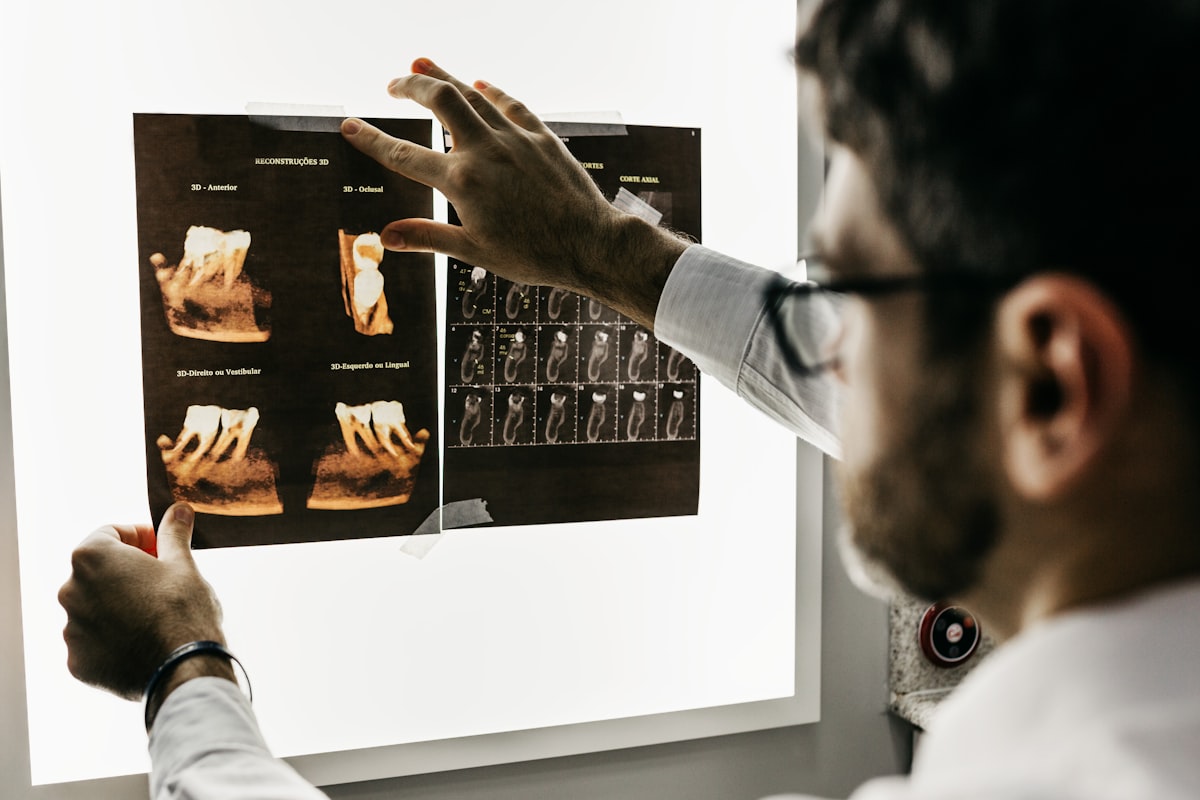
The mechanism relies on deep convolutional neural networks (CNNs). These sophisticated algorithms analyze pixel-level variations in radiopacity, comparing them against vast datasets of confirmed pathologies. Studies suggest that this technology is particularly adept at identifying early enamel demineralization, subtle periapical radiolucencies, and minute calculus deposits that often blend seamlessly into the surrounding anatomy.
How is error reduction accurately quantified?
The primary value proposition of AI in radiography is the mitigation of diagnostic errors. False negatives—where early decay is missed—often lead to more extensive and costly restorative work later. Conversely, false positives can result in unnecessary invasive procedures.
Recent longitudinal trials indicate that the application of FDA-cleared AI software acts as a powerful standardizing force. When clinicians utilize these tools, inter-examiner variability drops dramatically. In a multi-center study comparing human-only diagnostics to AI-assisted diagnostics, the AI-assisted group demonstrated a higher sensitivity for detecting interproximal lesions, particularly those confined strictly to the enamel layer.
By bounding these lesions with colored bounding boxes or probability scores on the screen, the software forces the clinician to pause and re-evaluate subtle shadows. Industry experts note that this "cognitive speed bump" is where the true value lies: it is not about replacing the dentist, but rather calibrating their focus.
What is the economic impact on clinical workflows?
Beyond clinical accuracy, the integration of AI radiography heavily influences practice economics and workflow efficiency. In a high-volume clinical environment, time is a scarce commodity. Automating the initial scan of a full-mouth series allows practitioners to allocate more time to patient communication and treatment planning.
Enhancing Patient Communication
One of the most consequential, yet under-discussed, benefits of AI in 2026 is its role in patient communication. Historically, explaining a subtle shadow on a black-and-white radiograph to a layperson has been a persistent challenge. Patients often struggle to see what the dentist sees, which can breed skepticism regarding proposed treatment plans.
AI platforms address this friction elegantly. By casting brightly colored overlays onto the X-rays—marking decay in red, calculus in yellow, and bone loss margins in green—the pathology is made irrefutably visible to the patient. Industry reports indicate that clinics utilizing these visual aids experience a measurable increase in case acceptance rates. Transparency builds trust, and algorithmic overlays provide an objective, third-party visualization that patients readily understand.
Administrative and Insurance Efficiencies
The backend operations of a modern dental practice also stand to benefit. Dental insurance claims processing frequently hinges on the subjective interpretation of radiographs by insurance adjusters. AI is beginning to standardize this discourse. When a claim includes an AI-annotated image alongside the clinical narrative, it provides a layer of objective data that can expedite the approval process.
Some forward-looking insurance groups are already adopting identical machine learning models on their end to auto-adjudicate claims. The implication for 2026 is clear: clinics that speak the "algorithmic language" of the insurers will likely experience fewer claim denials and faster revenue cycles.
Navigating the Regulatory and Ethical Landscape
With profound technological capabilities comes the necessity for stringent regulatory oversight. As of 2026, the regulatory bodies governing medical devices have established clear frameworks for dental AI software.
The Standard of Care
The prevailing legal and ethical consensus is that AI serves as an adjunct, not a replacement. It is an "assistive diagnostic device." The final responsibility for diagnosing and prescribing treatment rests invariably with the licensed dentist. The software cannot legally diagnose; it can only highlight statistical probabilities.
This distinction is crucial for liability and patient safety. Institutions like the American Dental Association continue to emphasize the importance of clinical judgment. If an AI model flags a shadow as caries, but the dentist's tactile explorer and clinical assessment reveal sound enamel, the clinical assessment overrides the algorithm.
Algorithmic Bias and Data Diversity
A persistent challenge in the development of healthcare AI is algorithm bias. If a machine learning model is trained predominantly on radiographs from a narrow demographic pool, its accuracy may degrade when applied to broader populations with varying anatomical norms.
Leading software developers have spent the last few years diversifying their training datasets, ensuring representation across age groups, ethnicities, and geographic locations. Clinics evaluating new software are increasingly advised to inquire about the diversity of the underlying training data to ensure equitable diagnostic performance across their entire patient base.
The Future Trajectory: Beyond 2D Caries Detection
While the current spotlight is on 2D caries and calculus detection, the trajectory points toward much deeper integration.
CBCT and 3D Volumetric Analysis
Cone Beam Computed Tomography (CBCT) generates vast amounts of three-dimensional data—far more than the human eye can comprehensively analyze in a standard consultation window. In 2026, AI is beginning to segment CBCT volumes automatically. It can map the inferior alveolar nerve canal with precision, automatically measure airway volume for sleep apnea assessments, and segment singular tooth roots for complex endodontic planning.
Predictive Analytics
Looking toward the late 2020s, the frontier of radiographic AI is predictive analytics. Rather than merely diagnosing existing decay, future iterations of these models aim to predict the likelihood of future decay or periodontal breakdown based on historical radiographic progression and pattern recognition. By analyzing the rate of bone loss over five years of historical X-rays, for instance, the algorithm may project future mobility issues, allowing for proactive, preventative interventions long before irreversible damage occurs.
What are the concluding thoughts for clinicians?
The integration of machine learning into dental radiography represents one of the most significant leaps in diagnostic standard-of-care in the 21st century. By serving as an indefatigable analytical aid, these algorithms are reducing oversight, standardizing care across providers, and fostering a level of transparency that greatly enhances the patient-provider relationship.
However, technology remains a tool, not a practitioner. The efficacy of AI is ultimately bottlenecked by the clinician interpreting its insights. In the modern dental landscape, the most successful practices are those that harmonize the objective precision of machine learning with the nuanced, empathetic judgment of the experienced dental professional.
Editorial Sidebar Statement: The Dental Mail operates as an independent journalistic entity. The analysis provided herein is derived from aggregated industry data and peer-reviewed studies. It is not intended to serve as medical or diagnostic advice. Clinicians should refer to primary literature and regulatory guidelines when adopting new technologies.
Research Transparency
This report is synthesized from primary industry data and clinical archives. We prioritize transparency by citing the original sources used in our reporting.
The Dental Mail is a journalistic platform. Information is provided for industry intelligence and does not constitute medical advice.
The Executive Briefing
Join 40,000+ dental leaders receiving critical industry intelligence and clinical updates every Tuesday morning.
No spam. Unsubscribe anytime.